Main navigation
The College of Nursing's service mission focuses on applying our resources to improve health care for Iowans.
An important part of this endeavor involves extending our academic programs to students who are unable to move to Iowa City in order to advance their nursing education. Some of these students are practicing registered nurses, with families and jobs in communities across the state. Our RN-BSN and graduate programs that are offered online allow them to continue to work, providing nursing care in their communities while pursuing advanced nursing education. The professional development of these practicing nurses is key to expanding the breadth and depth of health care services available to Iowans.
The excellence of health care available to Iowans is directly influenced by the collaborative activities of the College of Nursing with nurses and other health care providers across the state. Through development of partnerships with nurses in facilities and agencies throughout Iowa, the newest research-based information is being implemented into care delivery at the local level. This improves the quality of care Iowans receive and enhances the equality of care available throughout the state.
Outreach Projects
RN-BSN Program
One of the goals of the Strategic Plan for the College of Nursing is to prepare the next generation of nursing leaders. This includes providing access to baccalaureate education for nurses throughout the state. Our RN-BSN program is offered to nurses who have graduated from a hospital-based diploma program or from an associate degree in nursing program from a community college. This educational offering has a two-fold impact: 1) the knowledge and skills gained through this education will increase nurses' ability to provide quality care to diverse patient populations with increasingly complex health care needs; and, 2) this education provides the needed preparation for nurses to pursue graduate education. Since the summer of 2005, our program has been delivered through an online format.
Anita Nicholson, PhD, RN, Associate Dean for Undergraduate Programs
Nurse Anesthesia Program
The University of Iowa's College of Nursing offers the only Doctor of Nursing Practice (DNP) in Anesthesia Nursing Program in the entire state with the purpose of educating nurse anesthetists to take care of Iowans. Our graduate program is designed for RNs with a minimum of a bachelor's degree in Nursing (BSN, BAN) who wish to pursue a career as a nurse anesthetist (CRNA) and prepares expert clinicians to be leaders for the profession of nurse anesthesia and the U.S. healthcare system. Our DNP Program is jointly sponsored by UI's College of Nursing and the Roy J. and Lucille A. Carver College of Medicine's Department of Anesthesia. It is accredited by the CCNE and COA. The U.S. News & World Report recently ranked the University of Iowa's nurse anesthesia program at No. 9 compared to all other public and private university programs in the United States.
Cormac O'Sullivan, PhD, CRNA, ARNP, Nurse Anesthesia Program Director
Psychiatric-Mental Health Nurse Practitioner Program
The goal of this program is to increase access to mental health services by increasing the nursing workforce. This program prepares Psychiatric-Mental Health Advanced Practice Nurses to manage the complexity of psychiatric problems, promote mental health and disease prevention, and counsel and refer clients. Psychiatric-Mental Health services are in great need throughout Iowa, particularly in rural areas, so we are increasing student enrollment and financial support in this program, as well as providing psychiatric continuing education courses to primary care Nurse Practitioner providers across the state.
Dan Wesemann, DNP, PMHNP-BC, ARNP, Clinical Assistant Professor and Director of the PMHNP DNP Program
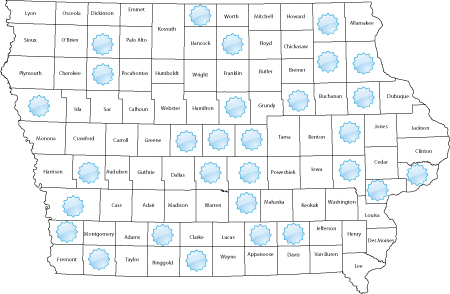
Cancer Pain in Elders Grant
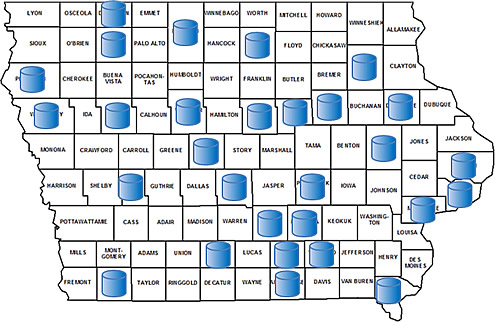
Cancer Pain in Elders: Promoting Evidence-Based Practices in Hospices is a six-year grant, funded by the National Cancer Institute, that focuses on promoting adoption of evidence-based practices to improve the quality of pain management for older adults with cancer in hospice. The study addresses barriers to consistent adoption of clinical practice guidelines for managing cancer pain in older adults. Translating Research into Practice (TRIP) is an active process of promoting use of evidence by health care providers. This study is evaluating the effect of an interdisciplinary, multifaceted TRIP intervention through selected activities that facilitate use of evidence-based practices for assessing and managing pain in older hospice patients with cancer. The study engages 16 hospices in the Midwest, 13 of which are in Iowa. The Iowa hospices provide services to patients in 53 of Iowa's 99 counties.
Keela Herr, PhD, RN, FAAN, AGSF, Professor, Associate Dean for Faculty
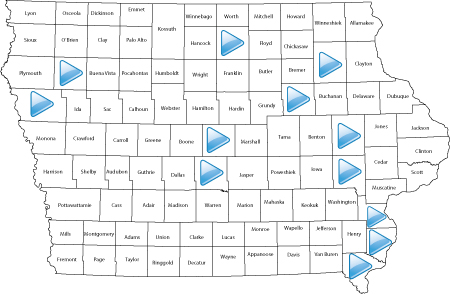
Train-The-Trainer: Maternal Depression Screening
Maternal depression affects approximately one in six women. Systematic screening increases the detection of maternal depression and is an important first step in getting women to treatment. The Train the Trainer: Maternal Depression Screening program disseminates maternal depression screening across the state of Iowa. Through the certification of 46 trainers in 29 counties across the state, maternal depression screening has been successfully implemented in many social service programs and hospital settings. Moreover, the certified trainers serve as local educational resources about perinatal depression.
Lisa Segre, PhD, Associate Professor
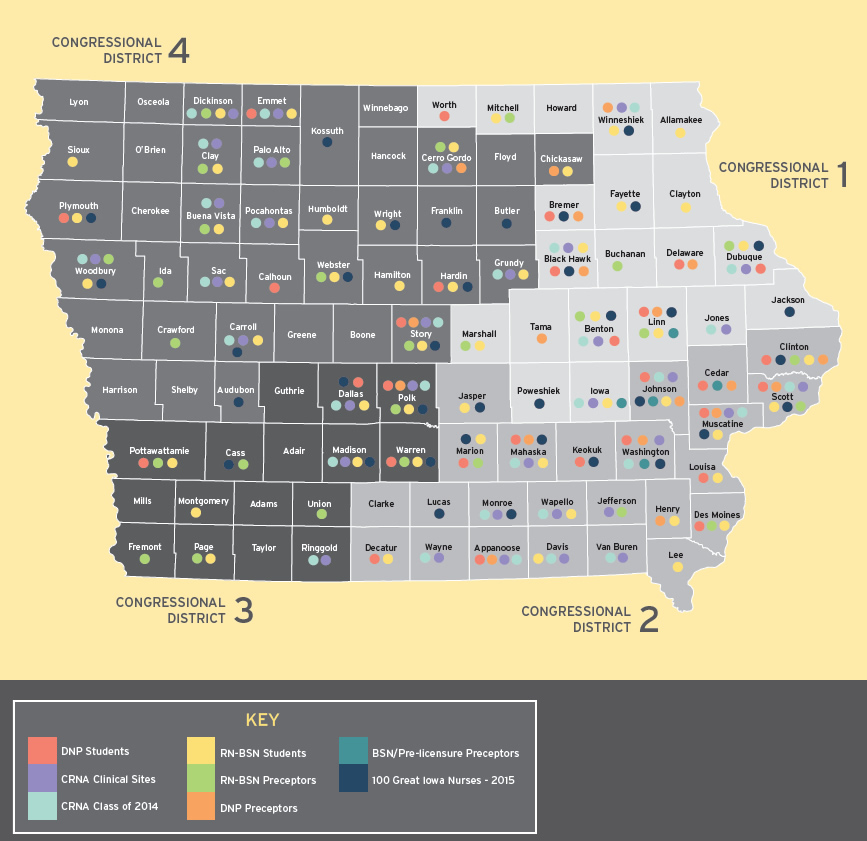
Improving Mood in Assisted Living Settings Using a Cognitive Training Intervention
Late-life depression levels are escalating, and include 24% of all tenants of Assisted Living (AL) settings. A promising, novel intervention is a computerized visual speed of processing training program known as Road Tour. Road Tour has been show to reduce depressive symptom levels and the risk of onset of clinical depression in community dwelling older adults. The investigators hypothesize that similar benefits will accrue to residents in AL settings. To evaluate this the investigators will use a two-arm, parallel, randomized controlled trial (RCT) comparing Road Tour training to attention control using computerized crossword puzzles among 300 adults 55 years old or older who reside in 15-30 AL settings that are partnering with the investigators.
The investigators hypothesize that Road Tour participants will have improved cognitive processing speed, lower levels of depressive symptoms, lower likelihood of the onset of clinical depression, less anxiety, lower levels of pain symptoms, and better health-related quality of life. These outcomes will be assessed at baseline, post-training, six months, and one year. The project is partnering with 28 AL settings from 12 different counties in Iowa.
Marianne Smith, PhD, RN, FAAN, Associate Professor
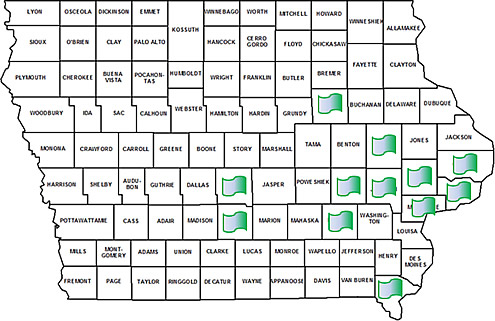
Preventing Persistent Post-Surgical Pain & Opioid Use in Veterans: Effect of ACT
A large number of veterans suffer from distress-based conditions, such as anxiety and depression, putting them at high risk of experiencing persistent pain and prolonged opioid use following surgery. These connections are based on strong and consistent evidence from the literature and our preliminary data. The proposed study adds a 1-day workshop of Acceptance and Commitment Therapy (ACT), followed by an individual "booster" session, to treatment as usual (TAU) to reduce veterans' risk of persistent pain and prolonged opioid use following surgery. ACT has been shown to be effective in reducing chronic pain, anxiety and depression. This pilot study will establish the feasibility and preliminary efficacy of incorporating ACT into treatment as usual (TAU) to preoperatively target distress-based risk factors. This project has attracted research participants from 15 different Iowa counties as well as from Illinois.
Barbara Rakel, PhD, RN, FAAN
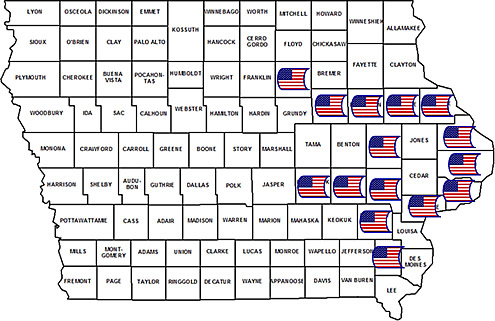
Vitamin D for Enhancing the Immune System in Cystic Fibrosis
Patients with Cystic Fibrosis (CF) have a shorter life span than the general population due to complications with lung infections, which eventually progress to lung failure. New research has suggested that high levels of vitamin D may be protective against lung infections and may promote the action of anti-bacterial proteins needed to ward off infections. Research has also suggested that high vitamin D levels are linked to lower mortality rates; however these hypotheses have not been adequately studied in patients with CF. An investigation of the effects of vitamin D supplementation is of particular interest in this population because patients with CF generally have high rates of vitamin D deficiency.
The investigators have preliminary data from a previous study suggesting that vitamin D supplementation in patients with CF lowers markers of inflammation, promotes anti-bacterial proteins, and reduces mortality. In this multi-center study funded by the Cystic Fibrosis Foundation Therapeutics, the investigators will examine the effects of a high dose vitamin D supplementation on patients with CF who are admitted to the hospital for lung infection. The PI of the study, Dr. Vin Tangpricha, MD, PhD, is at Emory University and the study also has sites in Alabama, Georgia, and Ohio as well as Iowa, where the project has recruited research participants from 6 different counties in Iowa.
Ruth Grossmann, PhD, RN, Assistant Professor (Site-PI)
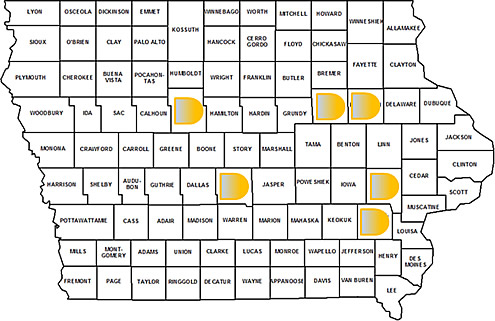
Organizational Trust & Nurse Report of Medication Errors
Medication delivery is a complex multistage process that involves several healthcare professionals. Medication errors occur at every step of the medication process, with 38% of errors occurring at the administration phase. It is estimated that average patient is subjected to at least one error per hospital stay day. Only 5 % of the errors are reported. Errors under-reporting is a major obstacle for quality and safety improvement initiatives.
The goal of the proposed project is to examine the role of organizational trust in enhancing nurses’ willingness to report medication errors. Organizational trust is one of the major organizational social capital assets; it has been linked to several organizational outcomes as commitment, job satisfaction and productivity. Organizational trust can be built and is strongly related to safety climate.
This study proposes that having high organizational trust in managers and peers can increase the nurses’ willingness to report medication errors. A sample of 350 RNs working in all inpatient medical-surgical and critical care units will be randomly selected from Iowa Board of Registered Nurses registry. Nurses represent 29 different counties across Iowa.
Containing the raising medication errors rates is a healthcare priority; improving medication errors reporting is vital for quality improvement initiatives. Findings from the present study will lay the groundwork for further studies that aim at designing intervention to enhance nurses’ willingness to report medication errors. This study will also add to the nursing body of knowledge as it will provide conceptual understanding to the concept of organizational trust.
Amany Farag, PhD, RN, Assistant Professor